Sleep Apnea Surgery
Sleep apnea surgery refers to a group of surgical procedures performed to address physical airway obstructions that contribute to obstructive sleep apnea (OSA). These procedures aim to reduce airway collapse during sleep by modifying specific anatomical structures, such as the nose, soft palate, jaw, or throat. Surgery is generally considered when non‑surgical options are not tolerated, not suitable, or when a clear anatomical cause has been identified.

Who May Benefit from Sleep Apnea Surgery
Individuals with Moderate to Severe OSA
Patients diagnosed with moderate to severe obstructive sleep apnea may be considered for sleep apnea surgery when breathing interruptions significantly affect sleep quality, daytime function, or overall health.
CPAP‑Intolerant Patients
Some individuals are unable to tolerate CPAP therapy due to discomfort, mask issues, or poor adherence. In such cases, surgical options may be explored after careful assessment.
Those with a Clear Anatomical Obstruction
Patients with structural contributors such as enlarged tonsils, nasal blockage, or jaw positioning issues may benefit when surgery directly addresses the site of obstruction.
People Seeking a Long‑Term Management Option
For selected individuals, sleep apnea surgery may form part of a longer‑term management plan, particularly when lifestyle measures and device‑based therapies are not feasible.
Who Should Avoid Sleep Apnea Surgery
Individuals with Uncontrolled Medical Conditions
Patients with poorly controlled heart, lung, or bleeding disorders may face higher surgical risks and require optimisation before considering surgery.
Those with Unrealistic Expectations
Surgery aims to reduce airway obstruction, but it may not completely resolve sleep apnea in all cases. Patients should have clear expectations and understand the role of surgery within a broader treatment plan.
Central or Mixed Sleep Apnea
Sleep apnea surgery is generally not suitable for central or mixed sleep apnea, where breathing disruption is related to neurological control rather than physical airway collapse.
How Sleep Apnea Surgery Is Performed
Consultation & Sleep Study
Assessment begins with a detailed clinical consultation, airway examination, and review of sleep study findings. These help identify obstruction sites and determine whether surgery is appropriate.
Procedure Selection & Planning
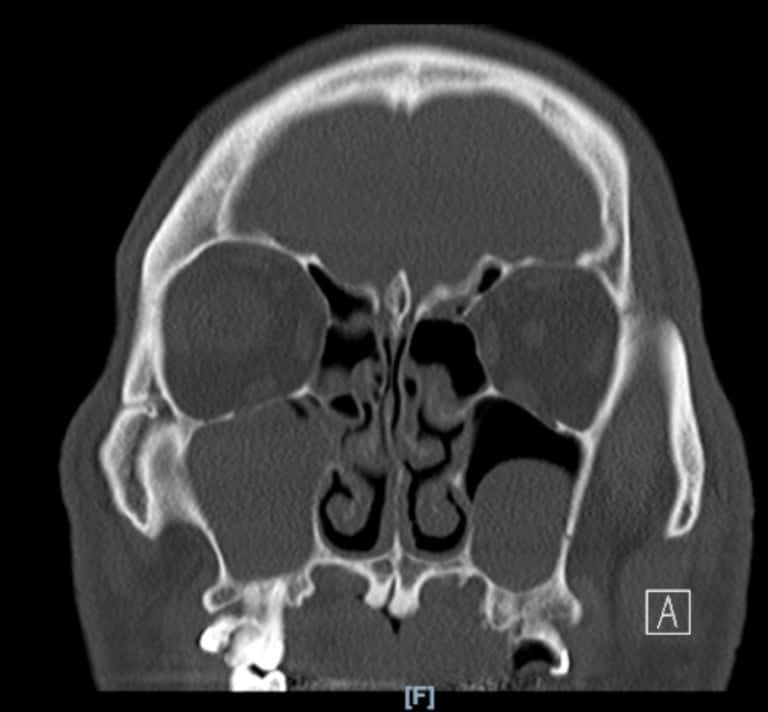
Surgical planning is individualised based on anatomy, severity of sleep apnea, and prior treatment response. Imaging or endoscopic evaluation may be used to guide decision‑making.
The Surgical Procedure
Palatal and Throat Surgery (UPPP)
Uvulopalatopharyngoplasty involves removing or reshaping excess tissue from the soft palate and back of the throat. This helps widen the airway and reduce collapse during sleep in selected patients with obstruction at this level.
Hypoglossal Nerve Stimulation
This procedure involves implanting a device that delivers electrical stimulation to the hypoglossal nerve during sleep. The stimulation encourages forward movement of the tongue, helping to maintain airway openness in suitable candidates.
Base of Tongue or Tonsil Reduction
When enlarged tonsils or a bulky tongue base contribute to airway blockage, targeted reduction may be performed using surgical or radiofrequency techniques to reduce tissue volume.
Maxillomandibular Advancement (MMA)
Maxillomandibular advancement is a more extensive procedure that repositions the upper and lower jaws forward to increase airway space. It is typically considered when jaw structure plays a significant role in airway narrowing.
Nasal Surgery
Procedures such as septoplasty or turbinate reduction address nasal obstruction that contributes to airflow resistance. Improving nasal breathing may reduce airway strain during sleep and improve tolerance of other therapies.
Tracheostomy
Tracheostomy creates a direct airway through the neck, bypassing upper airway obstruction entirely. This option is reserved for complex or severe cases where other treatments are not suitable.
Post‑Operative Monitoring
Following surgery, patients are monitored closely during the recovery period. Follow‑up reviews focus on healing, airway stability, symptom changes, and the need for additional treatment or ongoing support.
Schedule your consultation with Dr Dennis Chua for a diagnosis and personalised treatment options.
Risks and Side Effects of Sleep Apnea Surgery
Common Side Effects
Temporary pain, swelling, sore throat, nasal congestion, or difficulty swallowing may occur depending on the procedure performed.
Procedure‑Specific Risks
Different surgeries carry different risks, such as nasal bleeding after septoplasty or voice changes following throat surgery. These are discussed in detail during consultation.
Serious Risks (Rare)
As with any surgery, risks such as infection, bleeding, or adverse reactions to anaesthesia can occur, though these are uncommon.
Important Considerations
Surgery does not replace the need for follow‑up care. Some patients may still require additional therapies even after sleep apnea surgery.
Recovery and Aftercare After Sleep Apnea Surgery
Medical Monitoring and Communication
Regular follow‑up allows monitoring of healing, breathing patterns, and symptom changes. Patients are encouraged to report any concerns early.
Managing Common Side Effects at Home
Pain control, hydration, nasal care, and rest are important during the initial recovery phase. Instructions will vary depending on the procedure.
Lifestyle and Emotional Well‑Being
Recovery can take time. Adequate sleep, gradual return to activities, and emotional support play a role in post‑surgical adjustment.
Sleep Apnea Surgery Costs and Fees
Factors That Influence Cost
The cost of sleep apnea surgery depends on several factors, including the type of procedure performed, the complexity of the airway obstruction, anaesthesia requirements, and the choice of hospital or clinic setting. Additional costs may include pre-operative imaging, sleep studies, and post-operative follow-up.
Why Cost Varies
Each surgical plan is tailored to the individual. Some patients may require more than one procedure, while others may combine sleep apnea surgery with other treatments such as nasal or jaw surgery. As a result, fees will vary and are discussed during the consultation stage.
Cost Reduction and Support
Patients may explore insurance coverage, Medisave eligibility, or employer benefits. Cost considerations are discussed transparently during consultation.

Frequently Asked Questions
Is sleep apnea surgery a replacement for CPAP therapy?
Not always. Surgery may be considered when CPAP is not tolerated or when anatomical obstruction is present. In some cases, surgery and CPAP therapy are used together.
How do I know if surgery is suitable for me?
A detailed evaluation, including airway examination and sleep studies, is required. Consultation at an ENT clinic in Singapore helps determine if you are suitable.
Can surgery cure sleep apnea completely?
Results vary. Sleep apnea surgery aims to reduce airway obstruction, but some patients may still require additional treatment depending on underlying factors.
Is surgery suitable for snoring without sleep apnea?
Surgery may be considered in selected cases, but not all snoring requires surgical intervention. Learn more about snoring and how it differs from sleep apnea.
What’s the difference between sleep apnea and snoring?
Snoring involves vibration of airway tissues, while sleep apnea includes pauses in breathing.
How long is the recovery period?
Recovery time depends on the procedure performed. Some surgeries require a few weeks of healing, while others involve shorter downtime.
Contact Form
Feel free to contact, We are more than happy to assist you! We will get back to you as soon as possible.